 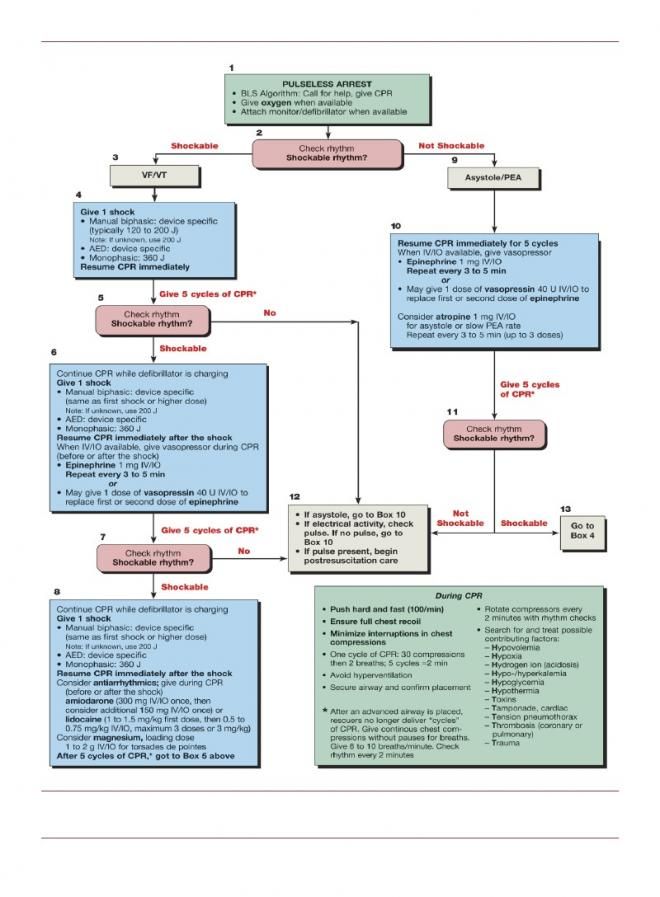
Within 24 hours before start of ED encounter or during ED encounter: Known structural cerebral vascular lesion (e.g., arteriovenous malformation) Known malignant intracranial neoplasm (primary or metastatic) Bleeding or bleeding diathesis (excluding menses) Allergic reaction to alteplase, streptokinase, anistreplase, tenecteplase, or reteplase Known structural cerebral vascular lesion (e.g., AVM).Known malignant intracranial neoplasm (primary or metastatic).Bleeding or bleeding diathesis (excluding menses).Cardiopulmonary arrest, including: cardiac arrest, CPR, defibrillation, respiratory arrest, or ventricular fibrillation (V-fib), ventricular tachycardia (VT), or pulseless electrical activity (PEA) or, traumatic or prolonged (>10 minutes) CPR.Intubation, including endotracheal intubation, mechanical ventilation, nasotracheal intubation, or orotracheal intubation.Mechanical circulatory assist device placement, including: aortic balloon pump, biventricular assist device, intra-aortic balloon, intra-aortic balloon counterpulsation, intra-aortic counterpulsation balloon pump, left ventricular device, percutaneous ventricular assist device, or ventricular assist device.Within 24 hours before start of ED encounter and during ED encounter: Within 21 days before end of ED encounter: Significant facial and/or closed head trauma.Within 90 days before start of ED encounter: Allergic reaction to alteplase, streptokinase, anistreplase, tenecteplase, or reteplase.Patients with the following conditions are excluded from measure denominator: Percentage of emergency department (ED) encounters for patients 18 years and older with a diagnosis of ST-segment elevation myocardial infarction (STEMI) that received appropriate treatment, defined as fibrinolytic therapy within 30 minutes of ED arrival, percutaneous coronary intervention (PCI) within 90 minutes of ED arrival, or transfer within 45 minutes of ED arrivalĪll emergency department encounters for patients 18 years and older at the start of the encounter with a diagnosis of ST-segment elevation myocardial infarction (STEMI) during the measurement periodĪll emergency department encounters for patients 18 years and older at the start of the encounter with a diagnosis of ST-segment elevation myocardial infarction (STEMI) during an Emergency Department encounter that ends during the measurement period No commercial use is permitted unless otherwise expressly granted.Appropriate Treatment for ST-Segment Elevation Myocardial Infarction (STEMI) Patients in the Emergency Department (ED) 
© Article author(s) (or their employer(s) unless otherwise stated in the text of the article) 2019. Sixteen (30%) piglets remained bradycardic (defined as HR of <100/min) after 10 min of asphyxia, identified by CBF, ECG and auscultation.Ĭlinicians should be aware of the potential inaccuracy of ECG assessment during asphyxia in newborn infants and should rather rely on assessment using a combination of auscultation, palpation, pulse oximetry and ECG.Īuscultation electrocardiography heart rate neonatal resuscitation newborn. In 23 (43%) piglets, we observed no CBF and no audible heart sounds, while ECG displayed an HR ranging from 15 to 80/min. In 14 (26%) piglets, CBF, ECG and auscultation identified asystole. Overall, 54 piglets were studied with a median (IQR) duration of asphyxia of 325 (200-491) s. Asystole was defined as zero carotid blood flow and was compared with ECG traces and auscultation for heart sounds using a neonatal/infant stethoscope. The piglets were exposed to 30 min normocapnic alveolar hypoxia followed by asphyxia until asystole, achieved by disconnecting the ventilator and clamping the endotracheal tube. This set-up allowed simultaneous monitoring of HR via ECG and carotid blood flow (CBF). Neonatal piglets had the right common carotid artery exposed and enclosed with a real-time ultrasonic flow probe and HR was continuously measured and recorded using ECG. To compare accuracy of ECG with auscultation to assess asystole in asphyxiated piglets. However, a recent case report raised concerns about this technique in the delivery room. The 2015 neonatal resuscitation guidelines added ECG as a recommended method of assessment of an infant's heart rate (HR) when determining the need for resuscitation at birth. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
